A nursing care plan for COPD is a comprehensive process that includes identifying the existing needs and evaluating potential risks.
Care plans are very helpful because they provide a means of communication among the patients, nurses, and healthcare providers to attain health care outcomes.
See also: How Can Nurses Improve Patient Outcomes?
In the absence of such a plan, the consistency and quality of patient care get lost.
Get to know more about the nursing care planning for COPD.
Table of Contents
Nursing care plan for a patient with COPD
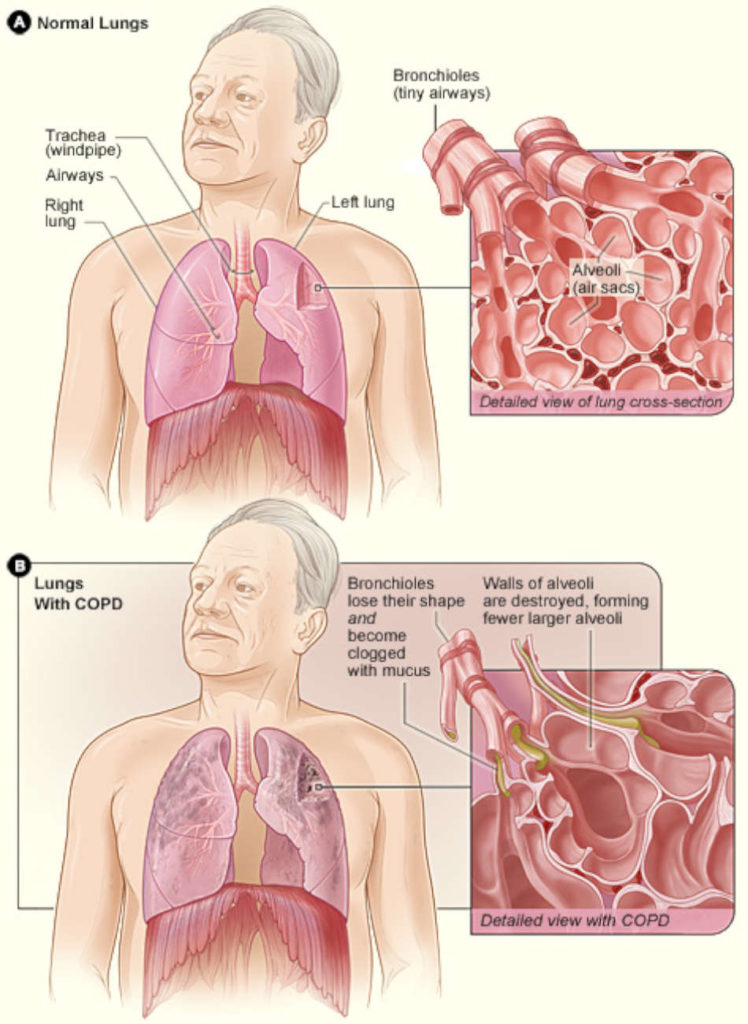
Nursing care planning for a patient with COPD includes the beginning of a treatment regimen to prevent complications and relieve symptoms.
Almost every patient with COPD receives outpatient treatment.
The nurses should have a teaching plan to help them understand the nature of this disease and comply with the therapy.
If the patient is regularly smoking, they need to quit soon.
Provide education on smoking and its benefit after quitting.
If the patient is finding it hard to breathe for longer periods and getting worse as time goes by, prepare with an airway cart.
Sometimes, the patient may be sedated and intubated to correct respiratory problems.
See also: Can Nurse Practitioners Intubate or Not?
Plan for oxygen monitoring with the help of a physician. Provide oxygen as needed.
In general, COPD patients need to be kept around 88% to 92%.
The heart and lungs are almost in the same area. If there is a problem in breathing, ensure that the heart is performing fine.
Even if the main problem is breathing, it is wise to monitor the heart. Hence, obtain an ECG.
Encourage the patient on attaining a healthy weight. Excess weight decreases the space for the lungs to function properly.
Also, patients who are thin have to get proper nutrition to maintain body performance.
As breathing gets difficult, patients find it harder to eat and breathe simultaneously.
Encouraging them to have smaller portions to eat and have frequent meals, ensures they aren’t lagging behind on nutrition.
A sedentary lifestyle can increase the frequency of shortness in breathing and have less tolerance for activities.
Help the patient by making them understand that movement improves breathing abilities.
Preventing pneumonia and influenza is important because the lungs are working hard to maintain the body’s carbon dioxide and oxygen levels.
See also: Nursing Care Plan for Pneumonia – Full Guide
The risk of an infection complicates the entire matter.
Nursing care plan for COPD exacerbation
Oral corticosteroids are not suited for normal maintenance treatment. But, oral corticosteroids play an important role during critical exacerbations.
Patients are given a short duration of tablets that lasts from 7 to 14 days.
Antibiotics could be necessary during exacerbation when the infection is suspended.
For instance, when the volume of darker sputum or sputum color is present.
National Institute for Health and Care Excellence (2018b) recommends oral antibiotic treatment in combination with clarithromycin, doxycycline, or amoxicillin.
Options for intravenous antibiotics may include co-trimoxazole, clarithromycin, co-amoxiclav, and piperacillin.
Routine sputum testing isn’t recommended, and poor response to these treatments may lead to changing the antibiotic.
Oral theophylline serves best for patients who cannot manage inhalers.
However, there is a very low agreement over its effectiveness in COPD.
A reduced dose may be helpful for patients with comorbidities. Mucolytic therapy is useful to patients who have a productive cough and struggles to expectorate effectively.
Prophylactic antibiotic treatment along with optimized inhalation therapy can be considered in some patients who have ongoing sputum production.
Also, this kind of therapy is suited for patients who don’t smoke but undergo four or more exacerbations per year, exacerbations that lead to hospital admission, or prolonged exacerbations.
Management of exacerbations:
- Optimizing bronchodilator medication is the first therapy. It helps in identifying the right medications or a few combinations of medications for a particular patient and taken on a regular schedule.
- Symptoms that indicate hospitalization intended for severe exacerbation of COPD may include critical dyspnea that isn’t capable of responding to the initial therapy, lethargy or confusion, paradoxical chest movement, peripheral edema, and respiratory muscle fatigue.
- After the patient arrives in the emergency room, oxygen therapy should be administered. Rapid assessment needs to be performed to find out whether the exacerbation could be life-threatening.
- Antibiotics are beneficial to patients who have increased sputum production, increased sputum purulence, and increased dyspnea.
Related articles of ours:
Nursing care plan for COPD ineffective airway clearance

The diagnosis of ineffective airway clearance may be defined as the incapacity to clear obstructions and secretions present on the respiratory tract so as to manage a clean airway.
See also: Can Nurse Practitioners Diagnose?
Breathing happens effortlessly and naturally to every human being.
But, some people are not capable to keep their airways clean and their lungs healthy.
It is very important to keep the airway clear and it has to be maintained well. If there is a problem in the airway, coughing takes place.
Coughing is the only way to clear the congested airway. But, coughing is not always easy for everyone.
Patients who are struggling with trauma, incisions, neuromuscular weakness, and respiratory muscle fatigue.
Mechanisms that are present in the lower alveoli and bronchioles to manage the flow in the airway include lymphatics, macrophages, and the mucociliary system.
Dehydration and anesthesia can change the functionalities of the mucociliary system.
See also: PACU Nurse Interview Questions
In this way, the increased production of secretions in medical conditions such as bronchitis and pneumonia can abuse these mechanisms.
IAC or ineffective airway clearance can be a chronic (spinal cord or CVA injury) or acute (postoperative recovery) problem.
Aged patients are the ones that have a higher risk of ineffective airway clearance.
See also: Nursing Care Plan for Constipation
Those individuals will have increased emphysema and a higher occurrence of sputum production or chronic cough.
There are plenty of airway clearance interventions that fall on the nursing care planning and nurses have the liberty to choose from them.
The nurses can choose the interventions while they are interacting with the patients and their family members about the strategies of secretion removal.
The nursing care plan for COPD helps to manage a clear airway, improve comfort while breathing, improve oxygenation and ventilation, and prevent risks connected with oxygenation issues.
See also: Nursing Care Plan for CVA
Conclusion: Nursing care plan for COPD
The nursing care plan for COPD begins after the patient gets admitted to the healthcare facility.
The plan is constantly updated throughout the period in response to the patient’s change in health conditions.
Planning and delivering patient-centered care is the starting point in nursing practice.
If you want to learn more about nursing care plans, check these articles of ours:
- Nursing Care Plan – Full Guide & Free Templates
- Nursing Care Plan for Diabetes
- Nursing Care Plan for Anxiety – Full Guide
- Nursing Care Plan Hypertension
- Nursing Care Plan for Pneumonia – Full Guide
- Nursing Care Plan for DVT – Full Guide
I’d also be glad if you could give this article a star rating down below. Thank you in advance!
